JACI:剖腹产、早产和食物过敏的风险相关研究
发布日期:2019-06-26
原标题:剖腹产、早产和食物过敏风险:瑞典全国100多万儿童群组研究
方法:这项瑞典全国性群组研究,使用了来自卫生保健登记簿中2001-2012年在瑞典出生的1086378名儿童的前瞻性记录数据。我们采用Cox回归分析,估计95%置信区间的危险比(HRs)于卫生保健登记簿中的围产期特征(如剖腹产和早产)和确诊的食物过敏之间的关系,并对婴儿性别和母亲因素进行了校正(分娩年龄、出生地、产次、吸烟、体重指数、哮喘/肺病)。
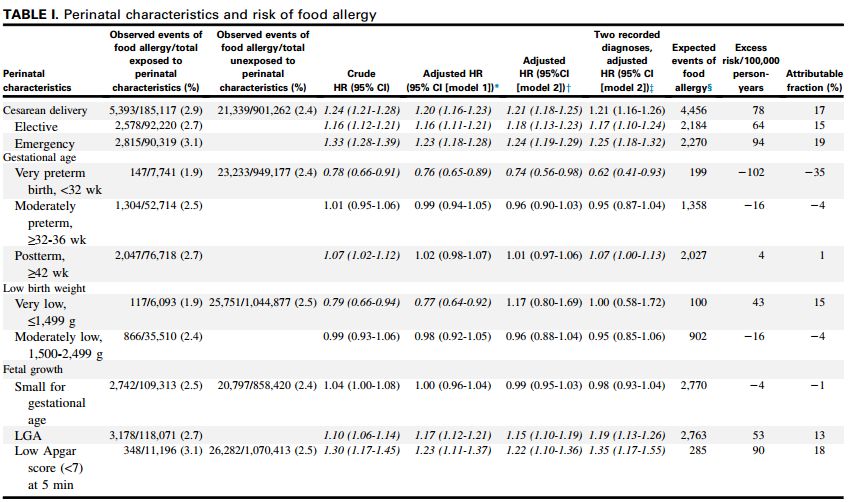
结果:在13年的随访中,26732名儿童(2.5%)被诊断为食物过敏。食物过敏与剖腹产(HR,1.21;95% CI,1.18-1.25)、胎龄大(HR,1.15;95% CI,1.10-1.19)和新生儿5分钟Apgar评分低(HR,1.22;95% CI,1.10-1.36)呈正相关,但与极早产(妊娠<32周:HR,0.74;95% CI,0.56-0.98)呈负相关。未发现食物过敏与中度早产、低出生体重或小于胎龄之间存在关联。当结果仅限于2个诊断食物过敏记录时,风险估计是相似的。1000名接受剖腹产的儿童与对照组相比,额外5名儿童出现食物过敏,这表明通过剖宫产出生的儿童中17%的食物过敏可以通过这种方式(归因分数)来解释。
结论:剖腹产与食物过敏风险增加相关,而极早产降低了风险。
延伸阅读
JACI
DOI: org/10.1016/j.jaci.2018.06.044
Abstract:
Background: Little is known about early-life risk factors for food allergy in children .
Methods: This nationwide Swedish cohort study of 1,086,378 children born in Sweden in 2001-2012 used prospectively recorded data from health care registers. Using Cox regression,we estimated hazard ratios (HRs) with 95% CIs for the association between perinatal characteristics (eg, cesarean delivery and preterm birth) and food allergy as defined by diagnoses in the National Patient Register, adjusting for infant sex and maternal factors (age at delivery, country of birth, parity, smoking, body mass index, and asthma/pulmonary disease).
Results: During the 13-year follow-up, 26,732 (2.5%) children were given a diagnosis of food allergy. Food allergy was positively associated with cesarean delivery (HR, 1.21; 95% CI, 1.18-1.25), large for gestational age (HR, 1.15; 95% CI,1.10-1.19), and low 5-minute Apgar score (HR, 1.22; 95% CI, 1.10-1.36) but negatively associated with very preterm birth (<32 weeks of gestation: HR, 0.74; 95% CI, 0.56-0.98). No association was found between food allergy and moderately preterm birth, low birth weight, or small for gestational age.Risk estimates were similar when the outcome was restricted to 2 records of diagnosed food allergy. In 1,000 children undergoing cesarean delivery, an extra 5 developed food allergy compared with the reference group, suggesting that 17% of food allergy in children born by means of cesarean delivery can be explained by this exposure (attributable fraction).
Conclusions: Cesarean delivery was associated with increasedrisk of food allergy, whereas very preterm birth decreased risk.
First Author:
Niki Mitselou
Correspondence:
Department of Pediatrics, Orebro University € Hospital, S€ odra Grev Rosengatan, Orebro 701 85, Sweden
All Authors:
Niki Mitselou, Jenny Hallberg, Olof Stephansson, Catarina Almqvist, Erik Melen, and Jonas F. Ludvigsson


——浙大迪迅 译
背景:我们对儿童生命早期食物过敏的危险因素知之甚少。方法:这项瑞典全国性群组研究,使用了来自卫生保健登记簿中2001-2012年在瑞典出生的1086378名儿童的前瞻性记录数据。我们采用Cox回归分析,估计95%置信区间的危险比(HRs)于卫生保健登记簿中的围产期特征(如剖腹产和早产)和确诊的食物过敏之间的关系,并对婴儿性别和母亲因素进行了校正(分娩年龄、出生地、产次、吸烟、体重指数、哮喘/肺病)。
结果:在13年的随访中,26732名儿童(2.5%)被诊断为食物过敏。食物过敏与剖腹产(HR,1.21;95% CI,1.18-1.25)、胎龄大(HR,1.15;95% CI,1.10-1.19)和新生儿5分钟Apgar评分低(HR,1.22;95% CI,1.10-1.36)呈正相关,但与极早产(妊娠<32周:HR,0.74;95% CI,0.56-0.98)呈负相关。未发现食物过敏与中度早产、低出生体重或小于胎龄之间存在关联。当结果仅限于2个诊断食物过敏记录时,风险估计是相似的。1000名接受剖腹产的儿童与对照组相比,额外5名儿童出现食物过敏,这表明通过剖宫产出生的儿童中17%的食物过敏可以通过这种方式(归因分数)来解释。
结论:剖腹产与食物过敏风险增加相关,而极早产降低了风险。

延伸阅读
JACI
[IF:13.258]
Cesarean delivery, preterm birth, and risk of food allergy: Nationwide Swedish cohort study of more than 1 million childrenDOI: org/10.1016/j.jaci.2018.06.044
Abstract:
Background: Little is known about early-life risk factors for food allergy in children .
Methods: This nationwide Swedish cohort study of 1,086,378 children born in Sweden in 2001-2012 used prospectively recorded data from health care registers. Using Cox regression,we estimated hazard ratios (HRs) with 95% CIs for the association between perinatal characteristics (eg, cesarean delivery and preterm birth) and food allergy as defined by diagnoses in the National Patient Register, adjusting for infant sex and maternal factors (age at delivery, country of birth, parity, smoking, body mass index, and asthma/pulmonary disease).
Results: During the 13-year follow-up, 26,732 (2.5%) children were given a diagnosis of food allergy. Food allergy was positively associated with cesarean delivery (HR, 1.21; 95% CI, 1.18-1.25), large for gestational age (HR, 1.15; 95% CI,1.10-1.19), and low 5-minute Apgar score (HR, 1.22; 95% CI, 1.10-1.36) but negatively associated with very preterm birth (<32 weeks of gestation: HR, 0.74; 95% CI, 0.56-0.98). No association was found between food allergy and moderately preterm birth, low birth weight, or small for gestational age.Risk estimates were similar when the outcome was restricted to 2 records of diagnosed food allergy. In 1,000 children undergoing cesarean delivery, an extra 5 developed food allergy compared with the reference group, suggesting that 17% of food allergy in children born by means of cesarean delivery can be explained by this exposure (attributable fraction).
Conclusions: Cesarean delivery was associated with increasedrisk of food allergy, whereas very preterm birth decreased risk.
First Author:
Niki Mitselou
Correspondence:
Department of Pediatrics, Orebro University € Hospital, S€ odra Grev Rosengatan, Orebro 701 85, Sweden
All Authors:
Niki Mitselou, Jenny Hallberg, Olof Stephansson, Catarina Almqvist, Erik Melen, and Jonas F. Ludvigsson
2019-01-17 Article
创建过敏性疾病的科研、科普知识交流平台,为过敏患者提供专业诊断、治疗、预防的共享平台。

 杭州浙大迪迅生物基因工程有限公司
杭州浙大迪迅生物基因工程有限公司

